PREVENTIVE TREATMENT IN MIGRAINE
Prof. Dr. F. Cankat Tulunay
Migraine is not merely a simple pain disorder characterized by episodic headache attacks. Today, migraine is accepted as a complex neurobiological disease associated with trigeminovascular system activation, neurogenic inflammation, cortical spreading depression, central sensitization, genetic predisposition, and disturbances in pain modulation pathways (1–3). The World Health Organization and Global Burden of Disease analyses define migraine as one of the leading causes of disability, particularly among young and middle-aged adults (4,5). The economic burden of migraine is not limited to medication costs alone; it is also associated with loss of workforce, presenteeism defined as being present at work but unable to work efficiently, decreased school performance, social isolation, depression, and serious deterioration in quality of life (5–7).
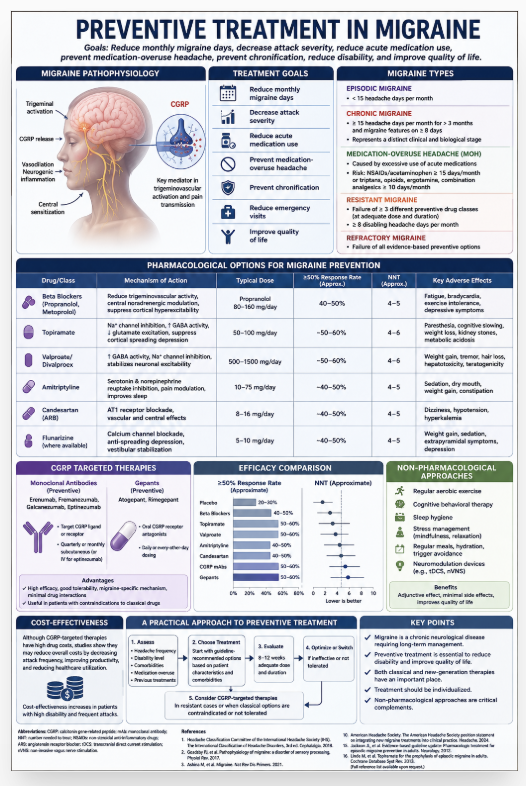
The aim of migraine prophylaxis is not only to reduce the number of attacks. In the modern approach, the goals are to reduce monthly migraine days, decrease attack severity, reduce acute medication use, prevent medication-overuse headache, prevent chronification, reduce emergency department visits, and restore the patient’s quality of life (8,9).
A major paradigm shift has occurred in migraine prophylaxis in recent years. For many years, beta blockers, antiepileptics, antidepressants, and calcium channel blockers were used as the main treatment options. However, with the development of CGRP-targeted monoclonal antibodies and gepants, the era of migraine-specific prophylaxis has begun (10,11). Nevertheless, classical drugs still maintain their importance. Today, the main debate is whether the newer drugs are truly superior to classical treatments, in which patient groups they should be preferred, and whether despite their high costs they actually reduce the overall economic burden.
MIGRAINE BIOLOGY AND CGRP PATHOPHYSIOLOGY
During a migraine attack, calcitonin gene-related peptide (CGRP), substance P, and other neuropeptides are released from trigeminal afferents. This process may lead to vasodilation of meningeal vessels, neurogenic inflammation, and increased pain transmission (2,3,10). CGRP plays a particularly important role in the maintenance of trigeminovascular system activation and central sensitization. Increased serum CGRP levels have been demonstrated during migraine attacks, and CGRP levels may decrease following triptan treatment (10,12).
For this reason, therapies targeting CGRP or the CGRP receptor are considered among the first migraine-specific prophylactic treatment groups. The 2024 position statement of the American Headache Society states that CGRP-targeted therapies may now be considered among first-line options for migraine prophylaxis, not only in resistant cases (10).
CHRONIC MIGRAINE AND MEDICATION-OVERUSE HEADACHE
According to ICHD-3, chronic migraine is defined as headache occurring on at least 15 days per month for more than three months, with migraine features present on at least 8 of those days (1). Chronic migraine does not simply mean more frequent attacks than episodic migraine; it represents a distinct clinical and biological stage. Central sensitization, persistent alterations in pain-processing pathways, and psychiatric comorbidities are more frequently observed in chronic migraine.
Medication-overuse headache is quite common in patients with chronic migraine. Medication-overuse headache is a chronic headache condition resulting from excessive use of acute headache medications (1). Use of NSAIDs and paracetamol for 15 or more days per month, or triptans, opioids, ergotamine, and combination analgesics for 10 or more days per month poses a risk. Approximately half of chronic migraine patients may have accompanying medication overuse (1,13).
RESISTANT AND REFRACTORY MIGRAINE
Resistant migraine is defined as the persistence of at least eight disabling headache days per month despite failure of at least three different prophylactic drug classes used at appropriate doses and durations. Refractory migraine refers to a more severe condition in which all currently evidence-based prophylactic options have failed (14). When evaluating resistant migraine, misdiagnosis, insufficient dosing, short treatment duration, medication overuse, sleep disorders, depression, anxiety, and treatment nonadherence must all be reviewed.
DRUGS USED IN MIGRAINE PROPHYLAXIS
Beta Blockers
Propranolol and metoprolol are among the most commonly used beta blockers in migraine prophylaxis. Although their mechanism of action is not fully understood, they are thought to reduce trigeminovascular system activity, provide central noradrenergic modulation, and suppress cortical hyperexcitability (8,9). Propranolol is generally used at doses of 80–160 mg/day. Meta-analyses report ≥50% response rates of approximately 40–50%, whereas placebo groups show response rates of approximately 20–30% (15). The NNT for propranolol is reported to be approximately 4–5. Major side effects include fatigue, bradycardia, exercise intolerance, and depressive symptoms. It should be used cautiously in asthma and severe bradycardia.
Topiramate
Topiramate is one of the classical drugs with the strongest evidence in migraine prophylaxis. It is thought to act through inhibition of voltage-dependent sodium channels, enhancement of GABA activity, reduction of glutamate excitation, and suppression of cortical spreading depression (16). It is generally started at 25 mg at night and titrated to 50–100 mg/day. Cochrane analyses have shown that topiramate significantly reduces migraine frequency compared with placebo and approximately doubles the ≥50% response rate (16). The NNT for topiramate is approximately 4–6.
However, tolerability problems with topiramate are important. Paresthesia, cognitive slowing, word-finding difficulty, reduced attention, weight loss, metabolic acidosis, and kidney stone risk may occur. In the HER-MES study, the rate of treatment discontinuation due to side effects in the topiramate group was approximately 39% (17).
Valproate and Divalproex
Valproate increases GABA levels and reduces neuronal excitability. Although effective in migraine prophylaxis, its use has become significantly restricted because of weight gain, tremor, sedation, hepatotoxicity, and especially teratogenicity (8,9). It should be avoided whenever possible in women of childbearing age.
Amitriptyline
Amitriptyline demonstrates serotonin and norepinephrine reuptake inhibition in addition to anticholinergic and antihistaminic effects. It may be particularly useful in patients with insomnia, depression, or accompanying tension-type headache. It is generally used at 10–75 mg/night. Sedation, dry mouth, weight gain, and orthostatic hypotension are common side effects.
Candesartan
Candesartan acts through angiotensin II type 1 receptor blockade. It may be useful in patients with hypertension or in those in whom sedative drugs are to be avoided. It is generally used at doses of 8–32 mg/day. Hypotension and hyperkalemia are side effects requiring attention.
Flunarizine
Flunarizine is a calcium channel modulator widely used in some countries. It may be beneficial in vestibular migraine and cases accompanied by dizziness. Because of side effects such as sedation, weight gain, depression, and parkinsonism-like symptoms, it should be used cautiously, especially in elderly patients.
CGRP Monoclonal Antibodies
Erenumab, fremanezumab, galcanezumab, and eptinezumab are CGRP-targeted monoclonal antibodies used in migraine prophylaxis (10,11). Erenumab targets the CGRP receptor, whereas the others target the CGRP ligand. Studies report ≥50% response rates of approximately 40–60%, whereas placebo response rates are generally around 20–35% (11).
Erenumab is generally administered subcutaneously at 70–140 mg monthly. In the HER-MES study, the ≥50% response rate was 55.4% with erenumab and 31.2% with topiramate. Treatment discontinuation rates were reported as 10.6% in the erenumab group and 38.9% in the topiramate group (17). These results are particularly noteworthy in terms of tolerability.
The major advantages of CGRP monoclonal antibodies are better tolerability, absence of sedation and weight gain, lower discontinuation rates, and migraine-specific targeted effects. Their disadvantages include high cost, reimbursement problems, still-limited long-term safety data, and insufficient pregnancy data.
Gepants
Atogepant and rimegepant are oral CGRP receptor antagonists. Atogepant is generally used at doses of 10–60 mg/day. Studies have shown significant reductions in monthly migraine days compared with placebo (18). The main side effects are nausea and constipation. The advantages of gepants are oral administration and migraine-specific mechanisms; however, long-term data are still limited.
OnabotulinumtoxinA
OnabotulinumtoxinA is used particularly in chronic migraine prophylaxis. The PREEMPT studies demonstrated significant improvement in headache days and quality-of-life measures in chronic migraine patients (19). In the PREEMPT protocol, doses of 155–195 units are generally administered every 12 weeks. Neck pain, local muscle weakness, and eyelid ptosis may occur.
ARE NEW DRUGS REALLY SUPERIOR TO CLASSICAL TREATMENTS?
The most important superiority of new drugs in migraine prophylaxis is often not absolute efficacy but rather tolerability and treatment continuation rates. Network meta-analyses show that classical drugs such as topiramate, beta blockers, valproate, and amitriptyline remain effective (20). However, CGRP monoclonal antibodies stand out because of lower discontinuation rates and better patient satisfaction.
Therefore, it cannot be said that new drugs are dramatically more powerful in every patient. Their real advantage lies in better tolerability, fewer systemic side effects, improved quality of life, and better adherence to treatment.
COMBINATION THERAPIES
Combination therapy is gaining increasing importance in migraine prophylaxis. Combination approaches may be considered particularly in chronic migraine, resistant migraine, or in cases with insufficient response to a single agent. Combinations such as topiramate plus beta blockers, amitriptyline plus beta blockers, or CGRP monoclonal antibodies combined with classical prophylactic agents may be used.
In recent years, the combination of CGRP monoclonal antibodies with onabotulinumtoxinA has attracted particular attention. Real-world data suggest that this approach may provide additional benefit in some resistant chronic migraine cases (21).
NON-PHARMACOLOGICAL METHODS
Non-pharmacological approaches are an integral component of migraine prophylaxis. These methods should not merely be viewed as “supportive recommendations”; in appropriately selected patients they may reduce attack frequency, decrease acute medication use, help avoid medication-related adverse effects, and in situations such as pregnancy, breastfeeding, childhood, advanced age, polypharmacy, or intolerance to classical prophylactic drugs, they may become central to treatment strategy.
However, the high placebo response in migraine must always be considered when evaluating non-pharmacological approaches. In migraine studies, the expectation of receiving treatment alone may significantly reduce headache frequency in some patients. Therefore, the true value of non-pharmacological interventions should be evaluated not only according to their benefits beyond placebo or sham procedures, but also in terms of low adverse-effect burden, long-term sustainability, and impact on quality of life.
Among behavioral treatments, the strongest evidence exists for biofeedback, relaxation training, and cognitive behavioral therapy. Biofeedback aims to increase awareness and partial voluntary control of physiological processes such as muscle tension, skin temperature, heart rate, and autonomic responses. It is particularly valuable in stress-triggered migraine, migraine associated with anxiety, pediatric and adolescent migraine, and in patients who should avoid medication use.
Studies report average reductions of approximately 40–50% in attack frequency with biofeedback and cognitive behavioral therapy. When combined with pharmacological treatment, success rates may approach 70% in some studies. An important advantage of these approaches is that the behavioral skills learned by the patient may continue to provide benefit even after treatment ends.
Cognitive behavioral therapy aims to modify the patient’s cognitive and emotional response to pain, strengthen stress management, and improve the ability to cope with triggers. Migraine patients frequently experience fear of impending attacks, catastrophic thinking, sleep disturbances, anxiety, and avoidance behavior. This psychological burden not only impairs quality of life but may also lower the pain threshold.
Relaxation training, diaphragmatic breathing, progressive muscle relaxation, meditation, and mindfulness practices may raise the migraine threshold by influencing autonomic nervous system balance. These methods are not miraculous when used alone; however, when combined with sleep regulation, exercise, trigger management, and if necessary pharmacological therapy, they may provide meaningful benefit.
Neuromodulation devices have emerged as noteworthy non-pharmacological options in migraine prophylaxis. Methods such as transcutaneous supraorbital nerve stimulation, non-invasive vagus nerve stimulation, and transcranial magnetic stimulation aim to modulate pain transmission and neuronal excitability by applying electrical or magnetic stimulation to the nervous system.
Nutraceuticals and supplements most frequently discussed include magnesium, riboflavin, and coenzyme Q10. Magnesium is thought to act through NMDA receptor activity, vascular tone, and neuronal excitability. Riboflavin may support mitochondrial energy metabolism, whereas coenzyme Q10 may exert effects through cellular energy pathways.
Lifestyle modification constitutes the foundation of migraine prophylaxis. The SEEDS approach provides a practical framework: regular sleep, regular exercise, regular eating habits, headache diary use, and stress management.
Acupuncture is among the most extensively studied complementary approaches in migraine prophylaxis. Cochrane reviews suggest that acupuncture may reduce attack frequency and in some studies may provide results comparable to prophylactic medications. However, sham acupuncture responses are also remarkably high.
SURGICAL METHODS IN MIGRAINE TREATMENT
Certain surgical procedures are performed under the terms “migraine surgery” or “migraine surgical treatment.” In recent years these methods have been heavily promoted on social media, in private clinics, and in some surgical centers. Nevertheless, migraine surgery remains a highly controversial field and is not currently accepted as routine standard migraine therapy in modern neurology guidelines.
The fundamental theory of migraine surgery is based on the assumption that in some migraine patients peripheral nerves may trigger the trigeminovascular system because of compression or irritation by surrounding tissues. According to this approach, surgical decompression of nerves such as the supraorbital, supratrochlear, occipital, or zygomaticotemporal nerves may reduce migraine attacks.
The work of plastic surgeon Bahman Guyuron played a major role in popularizing this field. Following observations that some patients experienced improvement in migraine symptoms after cosmetic forehead-lift procedures, the “trigger point surgery” concept was developed.
However, scientific controversies regarding migraine surgery are substantial. Modern migraine biology does not regard migraine as a disease explainable solely by peripheral nerve compression. Migraine is now understood as a complex neurobiological disorder involving central sensitization, trigeminovascular system activation, cortical spreading depression, CGRP release, and genetic predisposition.
Another major issue is the methodological limitations of surgical studies. Many studies involve small patient populations, lack sham controls, contain short follow-up periods, and remain vulnerable to strong placebo effects.
For this reason, migraine surgery should currently be regarded not as a proven standard therapy but as a controversial and still investigational approach that may be explored in carefully selected patients.
OCCIPITAL NERVE INJECTION
Occipital nerve injection involves the administration of local anesthetics, and sometimes corticosteroids, around the greater occipital nerve and occasionally the lesser occipital nerve located in the posterior scalp region. It is among the interventional procedures used particularly in chronic migraine, resistant migraine, occipital neuralgia, and certain other chronic headache syndromes.
The occipital nerves carry sensory innervation from the posterior scalp and are thought to interact with trigeminal pain systems. Current migraine biology recognizes close relationships between the trigeminovascular system and upper cervical neural structures.
Lidocaine or bupivacaine are commonly used local anesthetics. In some procedures corticosteroids such as methylprednisolone or triamcinolone may also be added.
Studies suggest that occipital nerve injections may reduce headache frequency, decrease pain severity, and lower acute medication use in some patients. Particularly in chronic migraine, symptom relief lasting from several weeks to several months has been reported.
However, occipital nerve injection is not considered a definitive or permanent treatment. It is currently regarded as an interventional supportive option that may benefit selected patients.
PREGNANCY, BREASTFEEDING, ELDERLY PATIENTS, AND CHILDREN
Migraine prophylaxis during pregnancy requires special caution. Drugs such as valproate and topiramate should be avoided whenever possible. Certain beta blockers and magnesium may be considered relatively safer options. Pregnancy data for CGRP monoclonal antibodies remain limited.
In elderly patients, polypharmacy, hypotension, fall risk, and cognitive adverse effects must be considered. Amitriptyline, flunarizine, and topiramate may create significant problems in older individuals.
Lifestyle modification is particularly important in pediatric and adolescent migraine. Placebo responses in children are generally higher than in adults.
REAL-WORLD DATA AND ACCESS PROBLEMS IN TÜRKİYE
Real-world data are important for understanding migraine prophylaxis in daily clinical practice. Real-world studies involving CGRP monoclonal antibodies generally report high patient satisfaction, low discontinuation rates, and marked improvement in quality of life.
In Türkiye, however, access to newer therapies remains a major problem. Because of reimbursement restrictions, high costs, limited access to neurologists, and delayed recognition of chronic migraine, many patients receive only acute analgesic treatment for years and appropriate prophylaxis is often initiated late.
CONCLUSION
Migraine prophylaxis has undergone a major transformation in recent years. While classical prophylactic medications continue to retain their importance, CGRP-targeted therapies and gepants have initiated the era of migraine-specific prevention.
The major advantages of newer treatments are better tolerability, lower discontinuation rates, and improved quality of life. Nevertheless, classical therapies have not disappeared entirely.
Today, the most appropriate approach is individualized prophylaxis based on migraine frequency, comorbidities, lifestyle, economic status, pregnancy plans, and treatment expectations.
REFERENCES
- Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 3rd edition. Cephalalgia. 2018;38:1-211.
- Goadsby PJ, Holland PR, Martins-Oliveira M, et al. Pathophysiology of migraine: a disorder of sensory processing. Physiol Rev. 2017;97:553-622.
- Ashina M. Migraine. N Engl J Med. 2020;383:1866-1876.
- World Health Organization. Headache disorders fact sheet.
- Global Burden of Disease Study 2021.
- Steiner TJ, Stovner LJ, Jensen R, et al. Migraine remains second among the world’s causes of disability. J Headache Pain. 2020;21:137.
- Lipton RB, Bigal ME. The epidemiology of migraine. Am J Med. 2005;118(Suppl 1):3S-10S.
- Diener HC, Holle D, Solbach K, Gaul C. Treatment of migraine attacks and prevention of migraine. Nervenarzt. 2022.
- Silberstein SD. Preventive migraine treatment. Neurol Clin. 2009;27:429-443.
- Charles AC, Digre KB, Goadsby PJ, et al. Calcitonin gene-related peptide-targeting therapies are a first-line option for migraine prevention. Headache. 2024;64:333-341.
- Sacco S, Amin FM, Ashina M, et al. European Headache Federation guideline on CGRP monoclonal antibodies. J Headache Pain. 2022;23:67.
- Edvinsson L. CGRP and migraine: from bench to bedside. Rev Neurol (Paris). 2021;177:785-790.
- Diener HC, Holle-Lee D, Nägel S, Gaul C, Göbel H. Medication-overuse headache: risk factors, pathophysiology and management. Nat Rev Neurol. 2016;12:575-583.
- European Headache Federation. Refractory migraine and resistant migraine consensus statement. J Headache Pain. 2020.
- Linde K, Rossnagel K. Propranolol for migraine prophylaxis. Cochrane Database Syst Rev. 2004.
- Linde M, Mulleners WM, Chronicle EP, McCrory DC. Topiramate for the prophylaxis of episodic migraine in adults. Cochrane Database Syst Rev. 2013.
- Reuter U, et al. Erenumab versus topiramate for the prevention of migraine — HER-MES trial. Cephalalgia. 2022.
- Ailani J, et al. Atogepant for the preventive treatment of migraine. N Engl J Med. 2021.
- Dodick DW, Turkel CC, DeGryse RE, et al. OnabotulinumtoxinA for treatment of chronic migraine: PREEMPT clinical program. Headache. 2010.
- Ferrari MD, et al. Migraine preventive drugs: systematic review and network meta-analysis. BMJ. 2023.
- Blumenfeld AM, et al. Real-world evidence for combination therapy with onabotulinumtoxinA and CGRP monoclonal antibodies in chronic migraine. Headache. 2022.







