BİONTECH VE MODERNA AŞILARI SPERM SAYISINI ARTIRIYOR.
ABD de Biontech ve Moderna aşısı olamak istemeyen %56 lık bir kesim aşıların doğurganlığı etkilediğine inanıyor. Bu aşıların klinik araştırmaları sırasında fertilite üzerine olan etkileri araştırılmadıysa da SARS-CoV2 virusunun sperm sayısını azalttığı gösterilmiştir. Bu çalışmada iki mRNA aşısının sperm sayısı üzerine etkileri araştırılmıştır.
Araştırma Miami Üniversitesinde 18-50 yaşlarındaki deneklerde yapılmış ve ilk doz aşıdan 2-7 gün önce ve son dozdan 90 gün sonra sperm sayıları ölçülmüştür.
Aşıdan önce Biontech grunda sperm sayısı 26 milyon, Moderna grubunda 36 milyon bulunmuştur. Son dozdan sonra Biontech grubunda sperm sayısı 30 milyona, Moderna aşısında 44 milyona yükselmiştir. Her iki grupta da hem sperm sayısı, hem sperm volümü anlamlı olarak artmıştır.
Enteresan olarak, aşıdan önce oligospermik (yetersiz sperm) olan 8 kişiden yedisinin sperm sayısı normale dönmüştür (8.5 milyondan 22 milyona yükselmiştir). Hiçbir denekte sperm sayısında azalma olmamıştır.
Sperm Parameters Before and After COVID-19 mRNA Vaccination
Daniel C. Gonzalez, BS1; Daniel E. Nassau, MD1; Kajal Khodamoradi, PhD1; et alEmad Ibrahim, MD1; Ruben Blachman-Braun, MD1; Jesse Ory, MD1; Ranjith Ramasamy, MD1
JAMA. 2021;326(3):273-274. doi:10.1001/jama.2021.9976
Two mRNA vaccines, BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna), received Emergency Use Authorization from the US Food and Drug Admin Miami istration. Despite high efficacy and few adverse events found in clinical trials, only 56% of individuals in the US reported wanting to receive the vaccine.1 One of the reasons for vaccine hesitancy is the potential negative effect on fertility.2 Because reproductive toxicity was not evaluated in the clinical trials and SARS-CoV-2 has been associated with decreases in sperm parameters,3 we assessed sperm parameters before and after mRNA vaccine administration.
Methods
This single-center prospective study at the University of Miami recruited healthy volunteers aged 18 to 50 years scheduled for mRNA COVID-19 vaccination through flyers posted throughout the university hospital and internal list-serve emails. The University of Miami institutional review board approved the study and written informed consent was obtained from all participants.
Men were prescreened to ensure they had no underlying fertility issues. Those with COVID-19 symptoms or a positive test result within 90 days were excluded. Participants provided a semen sample after 2 to 7 days of abstinence, prior to receiving the first vaccine dose and approximately 70 days after the second. Semen analyses were performed by trained andrologists per World Health Organization guidelines and included semen volume, sperm concentration, sperm motility, and total motile sperm count (TMSC).4 Individuals with oligospermia (sperm concentration <15 million/mL) were included. After calculating data distribution on normality test, medians and interquartile ranges (IQRs) were reported for all variables. The Wilcoxon rank sum test was used to compare pre- and postvaccination semen parameters. Change in TMSC is presented graphically. Statistical analysis was performed with SPSS version 24 (IBM). A 2-tailed P < .05 was considered statistically significant.
Results
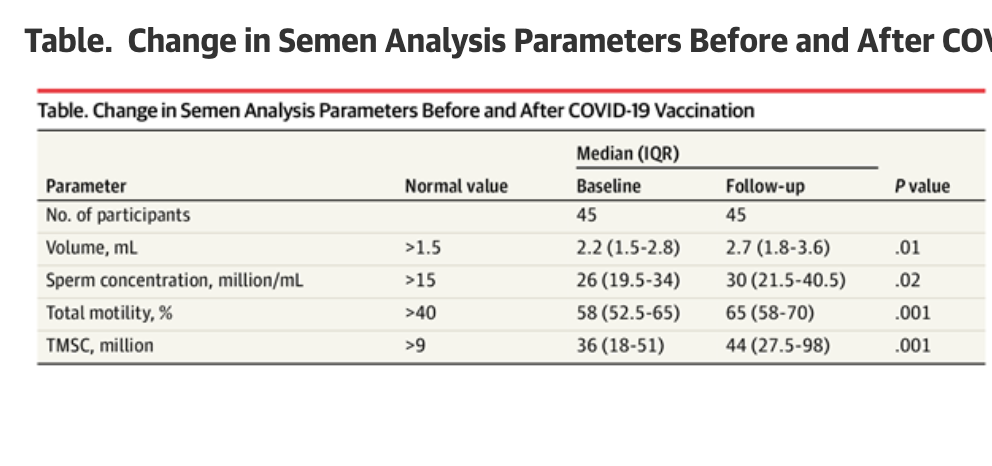
Between December 17, 2020, and January 12, 2021, 45 men volunteered (median age, 28 years [IQR, 25-31]); follow-up samples were obtained at a median of 75 days (IQR, 70-86) after the second dose. The study ended on April 24, 2021. Baseline samples were obtained after a median abstinence period of 2.8 days (IQR, 2-3) and follow-up samples after a median of 3 days (IQR, 3-4). Of the 45 men, 21 (46.7%) received BNT162b2 and 24 (53.3%) received mRNA-1273. Baseline median sperm concentration and TMSC were 26 million/mL (IQR, 19.5-34) and 36 million (IQR, 18-51), respectively. After the second vaccine dose, the median sperm concentration significantly increased to 30 million/mL (IQR, 21.5-40.5; P = .02) and the median TMSC to 44 million (IQR, 27.5-98; P = .001). Semen volume and sperm motility also significantly increased (Table).
Eight of the 45 men were oligospermic before the vaccine (median concentration, 8.5 million/mL [IQR, 5.1-12]). Of these 8, 7 men had increased sperm concentration to normozoospermic range at follow-up (median concentration, 22 million/mL [IQR, 17-25.5]), and 1 man remained oligospermic. No man became azoospermic after the vaccine.
The waterfall plot shows the within-participant change in TMSC from baseline (range, −22 million to 93 million) for each man (Figure).
Discussion
In this study of sperm parameters before and after 2 doses of a COVID-19 mRNA vaccine, there were no significant decreases in any sperm parameter among this small cohort of healthy men. Because the vaccines contain mRNA and not the live virus, it is unlikely that the vaccine would affect sperm parameters. While these results showed statistically significant increases in all sperm parameters, the magnitude of change is within normal individual variation and may be influenced by regression to the mean.5 Additionally, the increase may be due to the increased abstinence time before the second sample. Men with oligospermia did not experience further decline.
The limitations of the study include the small number of men enrolled; limited generalizability beyond young, healthy men; short follow-up; and lack of a control group. In addition, while semen analysis is the foundation of male fertility evaluation, it is an imperfect predictor of fertility potential. Despite this, the study’s time frame encompasses the full life cycle of sperm.
Section Editor: Jody W. Zylke, MD, Deputy Editor.
Article Information
Corresponding Author: Ranjith Ramasamy, MD, Department of Urology, University of Miami Miller School of Medicine, 1120 NW 14th St, 15th Fl, Miami, FL 33136 (ramasamy@miami.edu).
Accepted for Publication: June 1, 2021.
Published Online: June 17, 2021. doi:10.1001/jama.2021.9976
Author Contributions: Dr Ramasamy and Mr Gonzalez had full access to all of the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Concept and design: Gonzalez, Nassau, Ory, Ramasamy.
Acquisition, analysis, or interpretation of data: Gonzalez, Nassau, Khodamoradi, Ibrahim, Blachman-Braun.
Drafting of the manuscript: Gonzalez, Nassau, Khodamoradi, Blachman-Braun, Ory.
Critical revision of the manuscript for important intellectual content: Gonzalez, Nassau, Ibrahim, Blachman-Braun, Ory, Ramasamy.
Statistical analysis: Blachman-Braun, Ramasamy.
Administrative, technical, or material support: Gonzalez, Nassau, Khodamoradi, Ibrahim.
Supervision: Nassau, Ibrahim, Ory, Ramasamy.
Conflict of Interest Disclosures: None reported.
Additional Contributions: We thank Iakov Efimenko, BSc, Justin Dubin, MD, and Manuel Molina, MD (all with University of Miami Department of Urology), for assistance with recruitment and institutional review board preparation, as well as Ali Tourchi, MD (University of Arkansas for Medical Sciences Department of Urology), for developing the concept of the study. None were compensated for their contributions.
References
1.Szilagyi PGTK, Thomas K, Shah MD, et al. National trends in the US public’s likelihood of getting a COVID-19 vaccine: April 1 to December 8, 2020. JAMA. 2020;325(4):396-398. doi:10.1001/jama.2020.26419
ArticlePubMedGoogle ScholarCrossref
2.Berry SD, Johnson KS, Myles L, et al. Lessons learned from frontline skilled nursing facility staff regarding COVID-19 vaccine hesitancy. J Am Geriatr Soc. 2021;69(5):1140-1146. doi:10.1111/jgs.17136PubMedGoogle ScholarCrossref
3.Best JC, Kuchakulla M, Khodamoradi K, et al. Evaluation of SARS-CoV-2 in human semen and effect on total sperm number: a prospective observational study. World J Mens Health. 2021;39(e12).PubMedGoogle Scholar
4.Cooper TG, Noonan E, von Eckardstein S, et al. World Health Organization reference values for human semen characteristics. Hum Reprod Update. 2010;16(3):231-245. doi:10.1093/humupd/dmp048PubMedGoogle ScholarCrossref
5.Keel BA. Within- and between-subject variation in semen parameters in infertile men and normal semen donors. Fertil Steril. 2006;85(1):128-134. doi:10.1016/j.fertnstert.2005.06.048PubMedGoogle ScholarCrossref







